Our System...Your Training
Since 2002, Strategic Operations, Inc. (STOPS) has provided Hyper-Realistic® tactical training services and products to the military, law enforcement, first responders, and other organizations responsible for homeland security. STOPS pioneered the introduction of “Hollywood” style special effects and practices into live tactical training – explosions, weapons, realistic props, foreign language speaking actors, and casualty actors. Since the introduction of medical simulation systems such as the Cut Suit (CS) STOPS now offers Advanced Surgical Skills Packages (ASSP), which together are the world’s only Hyper-Realistic® open surgery simulator (CS-ASSP).
STOPS has added Hyper-Realistic® training support of civilian medical providers to its portfolio of products and services. STOPS continues to introduce innovative solutions to overcome the challenges of training military personnel, law enforcement personnel, first responders, and medical providers/surgical teams. STOPS is dedicated and focused on maximizing training value by outfitting individuals and organizations with essential training products to accomplish missions and save lives.
STOPS also provides Hyper-Realistic® training environments resembling actual scene conditions offering participants “Stress Inoculation.” Active threats and mass casualty incidents have been increasing in frequency and complexity throughout the United States – throughout the world, law enforcement and medical emergency response teams have struggled to manage actual events. A significant contributor to this reality is the way in which first responders are able to or unable to train for these incidents. Many lack the time, funding, and facilities to adequately prepare. STOPS draws upon many years of experience, since 2002, to provide a fully immersive training environment at the Tactical Training Lab in San Diego, CA or at any location throughout the world.

Hyper-Realistic® TrainingSTOPS defines Hyper-Realistic® as “such a high degree of fidelity in the replication of battlefield conditions in a training environment that participants so willingly suspend disbelief that they become totally immersed and eventually stress inoculated in a way that can be measured physiologically." All their senses tell them, emotionally and intellectually, that the scenarios are real. It is the ultimate in Theater Immersion Training. From point-of-injury to emergency room to surgical simulation. 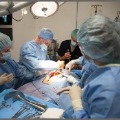
Medical SimulationThe Medical Simulation (MedSim) division is dedicated and focused on maximizing training value by outfitting medical providers with essential training products to accomplish lifesaving goals. By designing training products and medical simulation systems that are user-repairable, usage and cost effectiveness are maximized while minimizing out of service time for proprietary manufacturer repairs and costly replacement items. 
Construction & AtmosphericsThe legacy core of STOPS focuses on designing, fabricating, and constructing environments and training aids that are Hyper-Realistic® – and tactically challenging – by using Hollywood set construction techniques, combined with years of tactical training support experience. First responders receive mass casualty simulation training
CBS8 San Diego - January 20, 2024 
Being the Best @ AASTChicago, IL - September 21-24, 2022 The 81st Annual Meeting of American Association for the Surgery of Trauma (AAST) and Clinical Congress of Acute Care Surgery provided an opportunity for Strategic Operations, Inc. (STOPS) to demonstrate the features and capabilities of our medical simulation products and services. 
Strategic Operations Immersive Surgical and Trauma Skills Course week - KUSI News Coverage
May 2022 - Medical students experience Hyper-Realistic® training, exposing them to traumatic scenarios using the techniques of filmmaking special effects and make-up. Coupled with the patented wearable medical simulation aides from Strategic Operations Medical, the scenarios offer stress-inoculation for medical professionals and first responders.
As seen on the hit series 'DIRTY JOBS with MIKE ROWE' on Discovery and streaming on DiscoveryIn the season 9 finale (original air date February 6, 2022), Mike Rowe works alongside the talented people at Strategic Operations, Inc. who make innovative medical simulation products, like the world’s only Hyper-Realistic® Open Surgery Simulator, the Cut Suit. 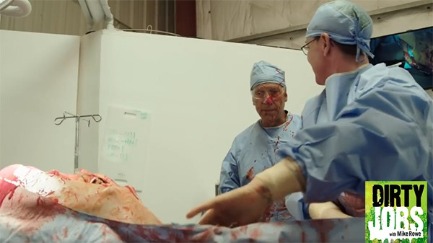
New York Health + Hospitals AAST Podium Presentation: HYPER-REALISTIC ADVANCED SURGICAL SKILLS PACKAGE WITH CUT SUIT SURGICAL SIMULATOR IMPROVES SURGERY TRAINEE CONFIDENCE IN OPERATIVE TRAUMA
September 29, 2021 - Michael Klein MD. of New York City Health + Hospitals. describes the dramatic results of a prospective, observational trial performed at the NYC H&H/Jacobi Institute for Medical Simulation and Advanced Learning (IMSAL) with surgical residents from 6 programs over two academic years using this innovative open surgery simulator.
|
|

















